Acne
Acne is a disorder of the skin marked by papules, comedones or cysts. Increased sebaceous activity or inflammation are often present as well.
Jump to
Acne/breakout-prone skin
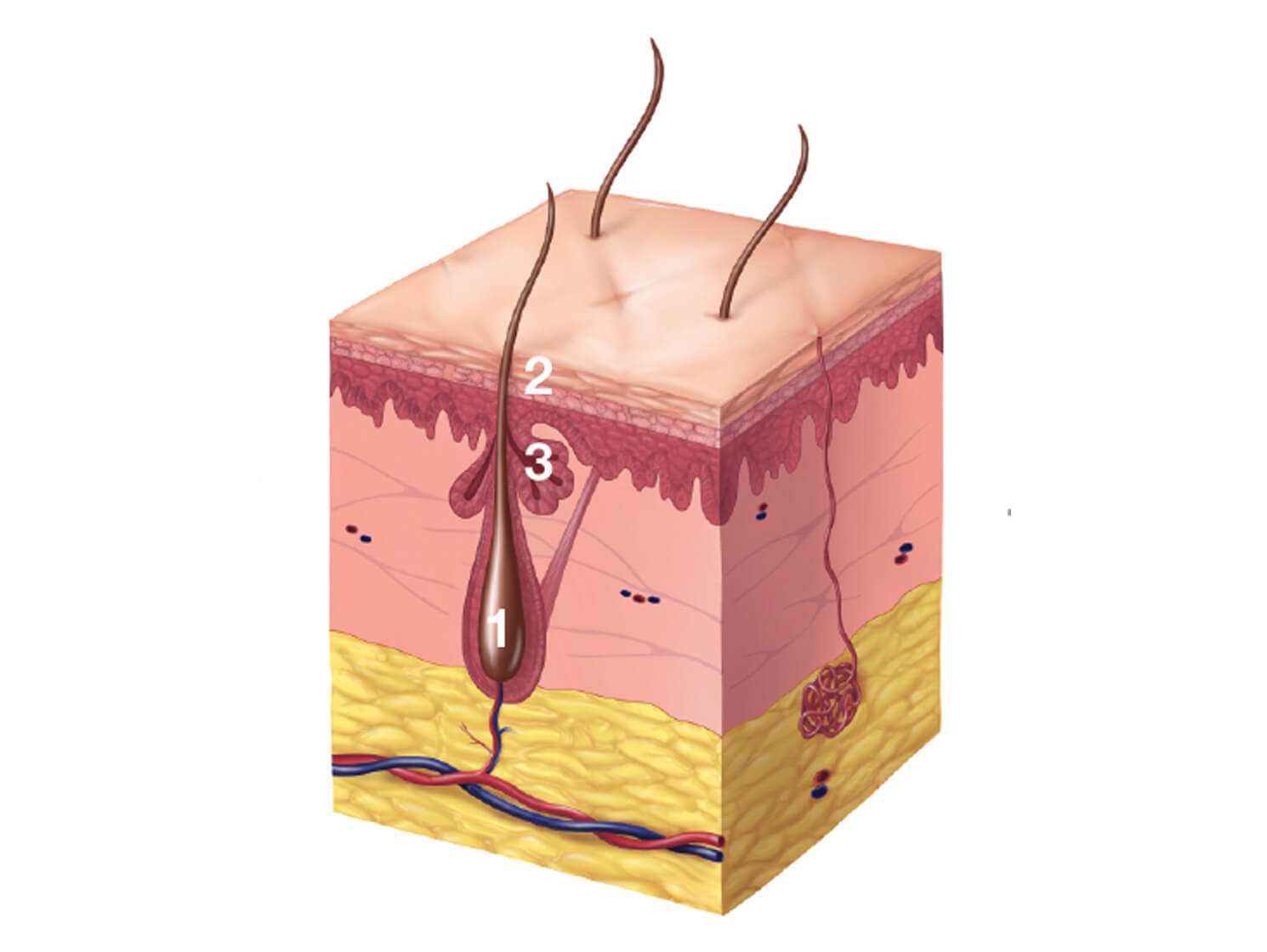
Normal follicle
- Hair follicle
- Open pore
- Sebaceous gland produces oily sebum

Closed comedone
Androgen hormones increase the adherence of keratinocytes to the follicle wall and increase sebum production, resulting in a plugged pore.
- Keratinocytes adhere to follicle wall
- Sebum production increases
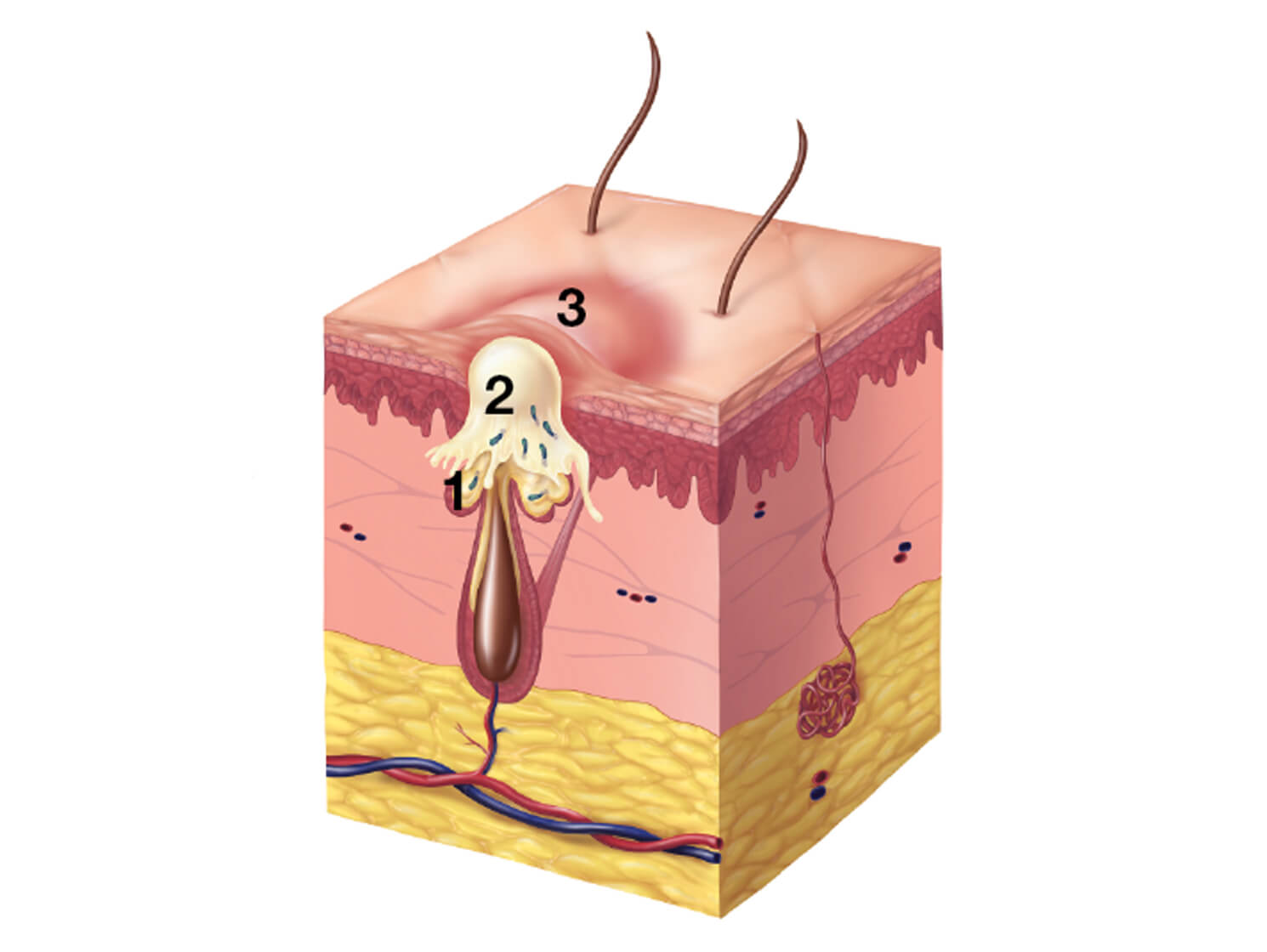
Papule
Increased sebum and P. acnes bacteria build up behind the plug and trigger an inflammatory response.
- Sebum increases
- Bacteria and sebum build up under the plug
- Inflammatory response
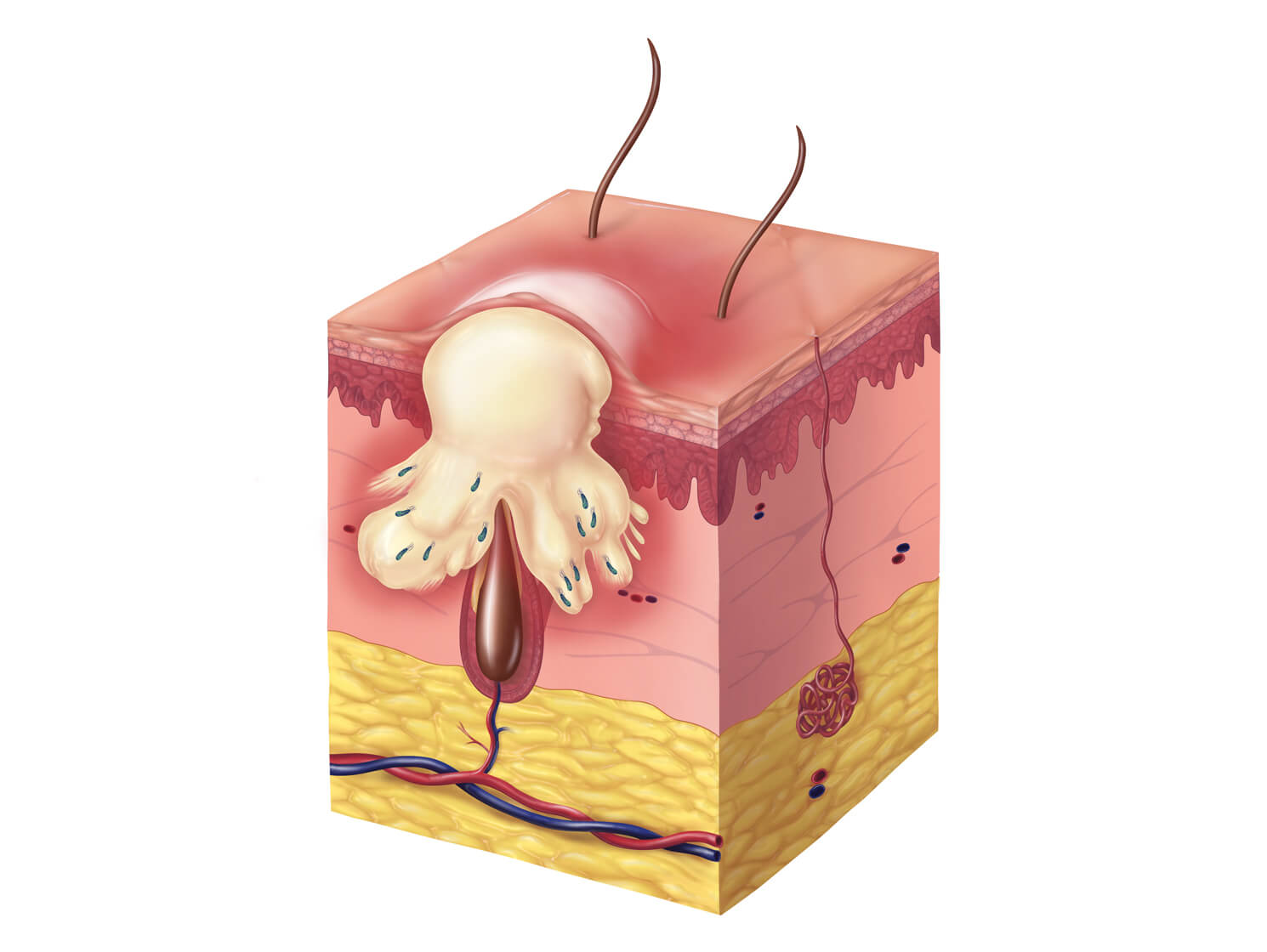
Pustule
The number of P. acnes increases, and breaks down sebum into irritating free fatty acids which stimulate an immune response. White blood cells weaken the follicular wall resulting in rupture and increased inflammation.
- P. acnes proliferates
- Follicle wall can rupture
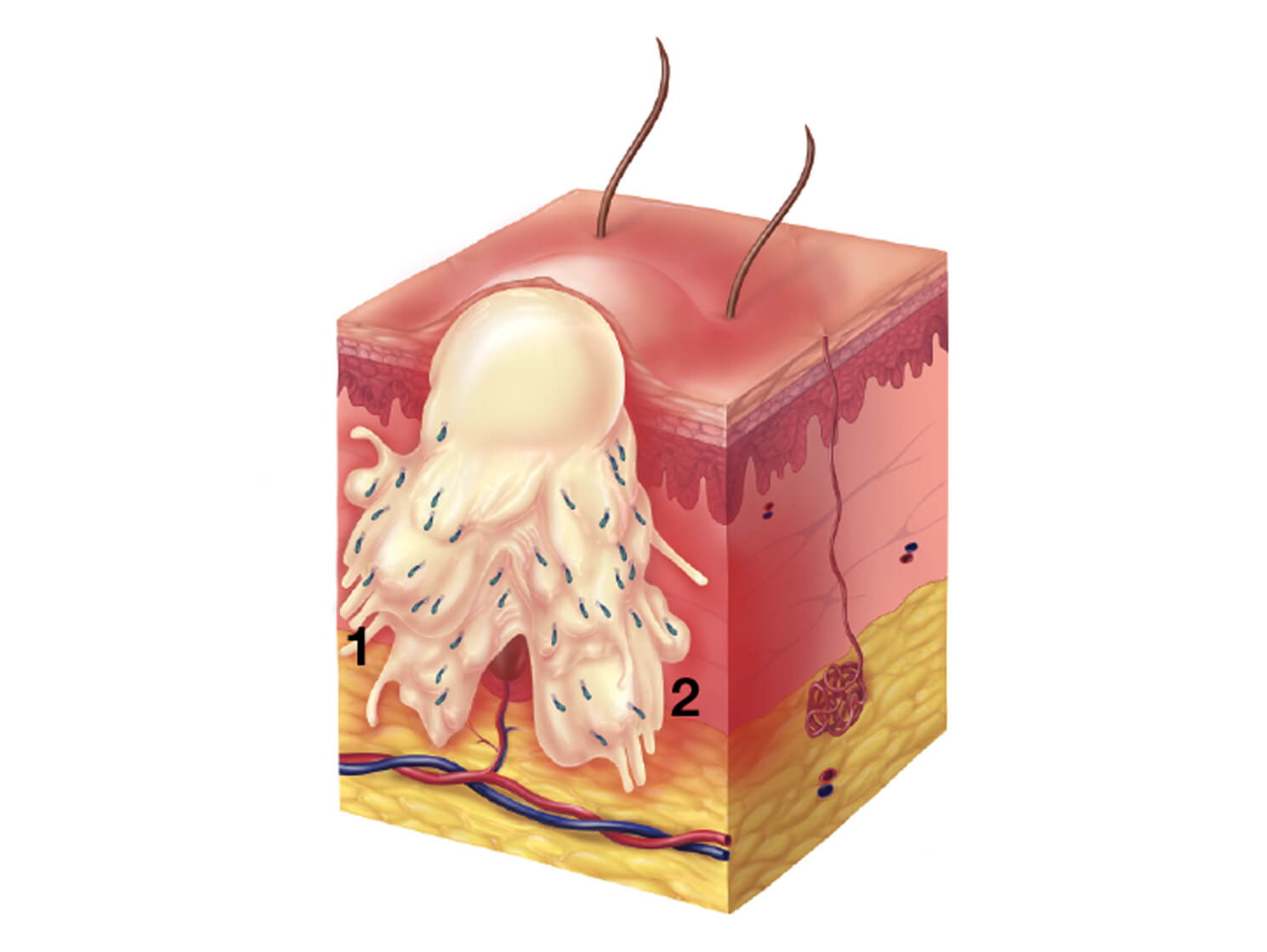
Nodule
Ruptures in follicle wall with marked inflammation and tissue destruction with possible scarring.
- Follicular wall ruptures
- Inflammation and tissue destruction
Types
& Causes
Acne
Grades of Acne
Acne simplex
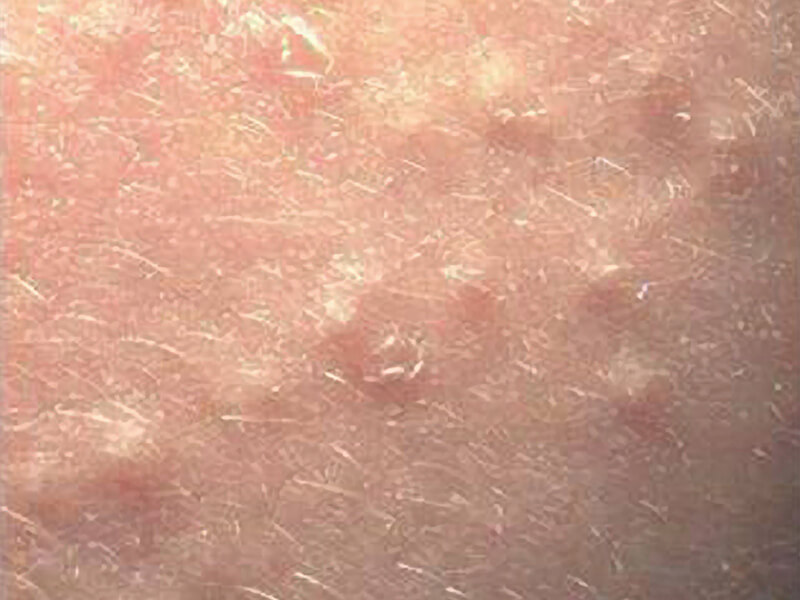
Grade I – considered acne simplex and may include open or closed comedones. Inflammatory lesions and cysts are not typically seen. Scarring is unlikely in acne simplex as the lesions tend to be superficial; however, patient excoriation may lead to hyperpigmentation or texture changes.
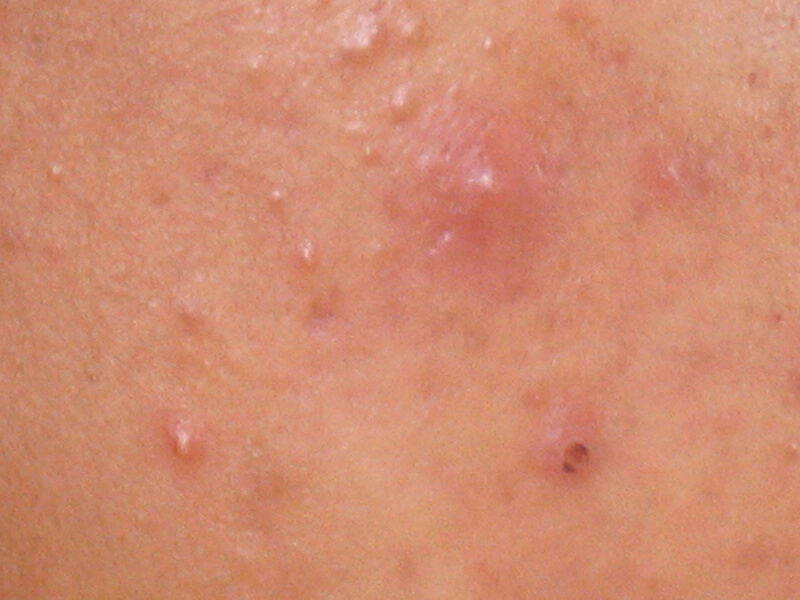
Grade II – also considered acne simplex and will include the open or closed comedones seen in grade I, as well as papules and pustules. Cystic lesions and scarring are uncommon.
Acne vulgaris
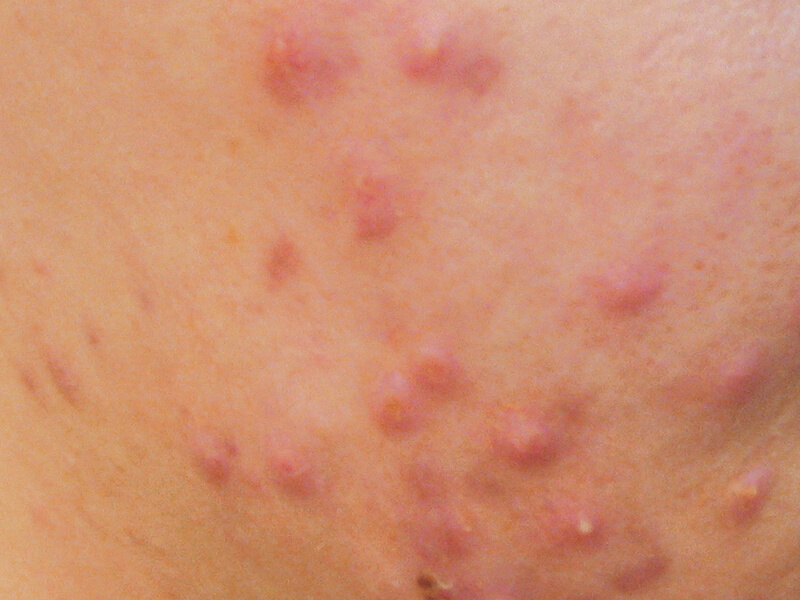
Grade III – a form of acne vulgaris, where inflammation and bacterial lesions are typical. Open and closed comedones may also be seen and scarring will be more likely than with the lower acne grades. Medical prescription intervention may be necessary.
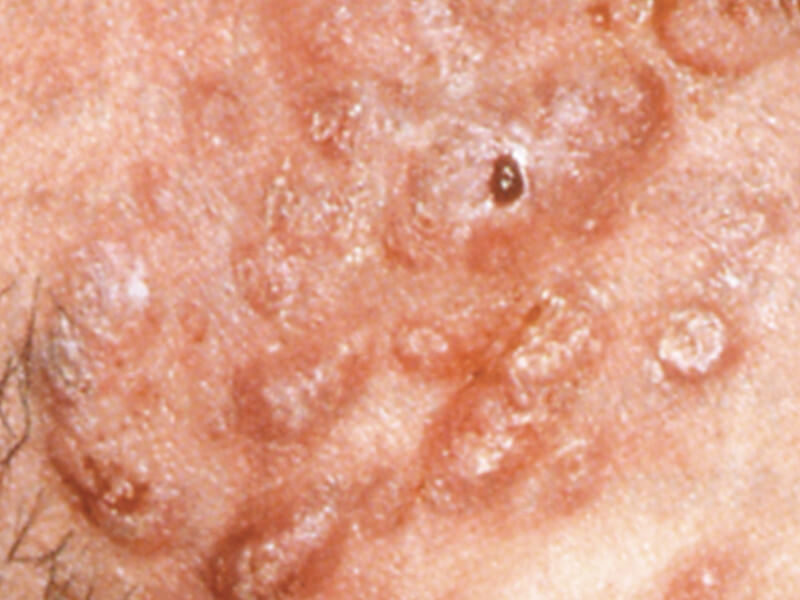
Grade IV – sufferers experience deeper cystic and nodular lesions, as well as papules, pustules and comedones. Scarring is very common due to the depth of the lesions. Medical prescription intervention is recommended.
Four main causes of acne
- increased keratinization within the follicle
- increased sebum production
- proliferation of Propionibacterium acnes (P.acnes) bacteria
- inflammation
Common presentations
- Hormonal acne is common in adolescence and is typically accompanied by an overproduction of sebum. Cyclical breakouts are often seen in females in the perioral area and hormonal acne may present itself at any stage in life when hormones fluctuate (e.g. pregnancy, introduction of oral contraceptives, menopause).
- Acne cosmetica is triggered by comedogenic or irritating ingredients in every day products. Certain makeup, laundry detergents, and hair care products may clog the pores and lead to breakouts. Regularly changing pillow cases and cleaning makeup applicators will help treat acne cosmetica.
- Inflammatory acne is red and inflamed, and may be uncomfortable for the patient. Asphyxiated acne is characterized by a rough surface keratolytic buildup and reduced cell turnover with sebum and other debris trapped beneath. Asphyxiated acne is more common in dry environments and may be caused by the use of drying ingredients, such as alcohol, without the use of a daily hydrator.
- Bacterial acne may be the result of an over-production of bacteria within the follicle or pore. P. acnes is the bacteria responsible for acne. It is anaerobic (cannot live in the presence of oxygen) and flourishes in warm, humid environments. Topical oxygen sources, such as benzoyl peroxide, help to control bacteria distribution and proliferation.
- Cystic acne sufferers experience large, painful nodules beneath the surface of the skin, which can remain for weeks or months. The depth and inflammation associated with cystic acne can destroy the follicle, resulting in scarring.
- Systemic acne usually appears as acne vulgaris, may involve other areas of the body (arms, chest, back, and shoulders) and may be brought on by disease, illness, medication, or other diet-related issues
Treatments
& Protocols
How to Treat
-
Acne: Gently Exfoliate and Increase Cell Turnover -
Acne: Control Sebum Production -
Acne: Decrease Propionibacterium Proliferation -
Acne: Protect from UV Rays and Other Inflammatory Stimulants
Professional Treatment Protocols
-
PCA Peel® Treatment Protocol -
Smoothing Body Peel® Treatment Protocol -
Ultra Peel® Treatment Protocol -
MD Peel (CCl3) Treatment Protocol -
Advanced Treatment Booster Protocol -
Therapeutic Mask Treatment Protocol -
Detoxifying Pore Treatment Protocol -
Oxygenating Trio® Treatment Protocol -
Sensi Peel® Treatment Protocol



